This article has been fact-checked by Dr Timothy Lim Yong Kuei, gynecologist at Timothy Lim Clinic for Women & Cancer Surgery, Mount Alvernia Hospital, Singapore.
About the Doctor
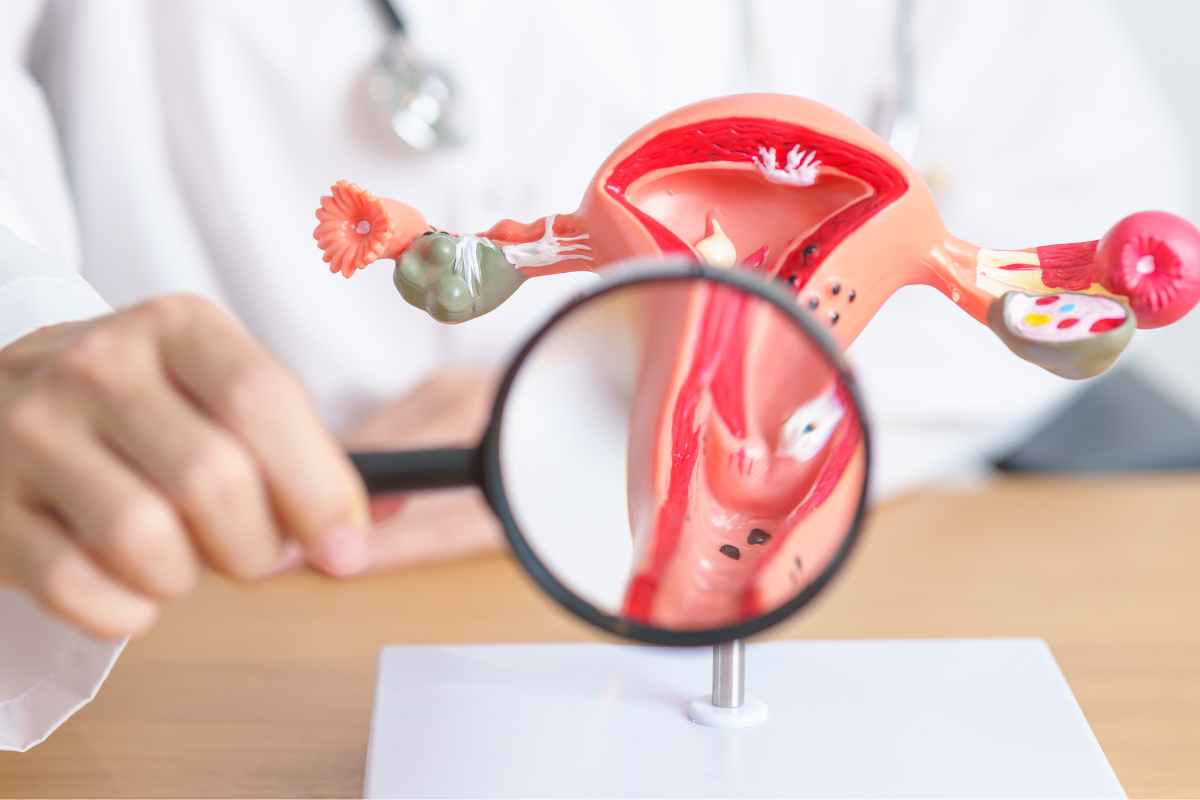
Human papillomavirus (HPV) is a common virus spread by skin-to-skin contact, usually during intercourse, though HPV infection is possible without sexual intercourse. There are different types of HPV; some types cause genital warts, like types 6 and 11, and are referred to as low-risk types as they are not linked to cancer. Other types of HPV, referred to as high-risk types, are linked to cancer, like types 16 and 18. These high-risk HPV types are associated with several cancers including cervical, anal, vaginal, penile, oral, and throat cancers. HPV infection usually causes no symptoms. For the majority of people, the immune system clears HPV before it can cause disease, such as genital warts and cervical cancer. In some cases, HPV infection is not cleared. If infected with a high-risk type of HPV, changes, called dysplasia, can occur in the cervical cells over 3-7 years, which can result in cervical cancer.
Cervical cancer is the 4th most common cancer affecting women, with 500,000 new cases annually worldwide. Early-stage cervical cancer often causes no symptoms, but if present, can include vaginal bleeding after intercourse, vaginal bleeding after menopause, bleeding between periods or heavier/longer periods, vaginal discharge with odour or containing blood, and pain during intercourse. Advanced-stage cervical cancer, once cancer has spread beyond the cervix, can cause rectal bleeding, pain with bowel movements, blood in the urine, painful urination, back pain, abdominal pain, fatigue, and leg swelling. HPV types, 16 and 18, are the most common types linked to invasive cervical cancer, though 20 HPV types have been associated with cancer.
Cervical cancer is preventable through screening and vaccination interventions. The World Health Organization (WHO) recommends primary screening with HPV DNA testing using a “screen-and-treat approach” or a “screen, triage, and treat approach” for the general population. In the “screen-and-treat approach”, those who are HPV positive are treated. In the “screen, triage, and treat approach”, primary screening with HPV DNA testing is first completed. If HPV-positive, a secondary test is performed, such as HPV partial genotyping, colposcopy, visual inspection with acetic acid (VIA), or cytology to triage those who require treatment. Individuals with a positive primary and secondary test undergo treatment. Regular cervical cancer screening every 5-10 years, starting at the age of 30, up to age 50, when using HPV DNA testing is recommended. If HPV DNA testing is not available, regular screening with VIA or cytology is recommended every 3 years. Screening can be stopped after the age of 50, provided there have been two consecutive negative screening results.
Another way to prevent cervical cancer is through the HPV vaccine. The HPV vaccine is safe and can reduce the risk of HPV-related genital warts and cancer by 99% and is highly effective when given before becoming sexually active. Those who are already sexually active can still receive the HPV vaccine. Those with an HPV infection and cervical dysplasia may receive the HPV vaccine to help prevent abnormal cells from recurring after treatment. Currently, there are 6 licensed HPV vaccines available, all of which offer protection against the high-risk HPV types 16 and 18, which are the cause of about 70% of cervical cancer cases in the world. The HPV vaccine is typically administered from ages 9-26, and can be used up to age 45. Even after receiving the HPV vaccine, regular cervical cancer screening is still recommended. The WHO recommends the following HPV vaccine schedule, according to age, in the general population.
- A 1-2 dose schedule for girls aged 9-14
- A 1-2 dose schedule for girls and women aged 15-20
- 2 doses with a 6-month interval for women older than 21