General Surgery
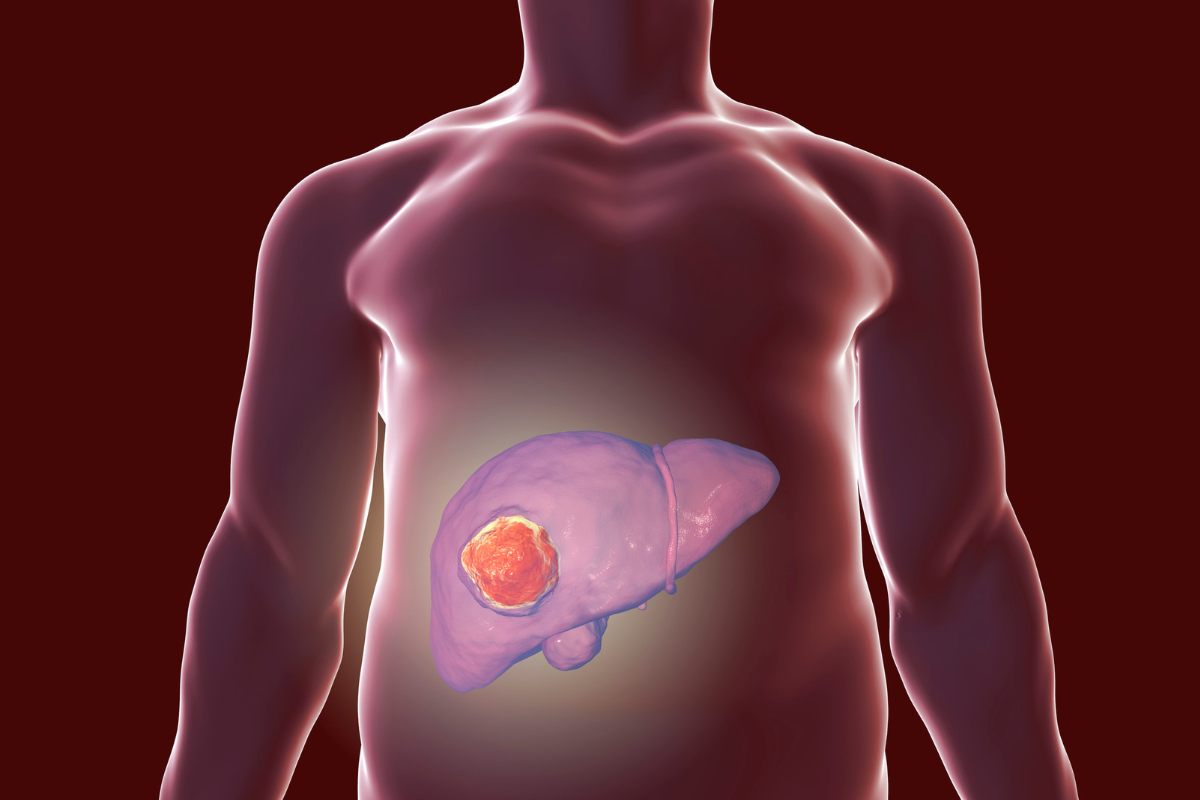
Keyhole Surgery for Liver Cancer
Keyhole surgery, also known as laparoscopic surgery, is a minimally invasive surgical technique used in various medical fields, including the treatment of liver cancer.
This article has been fact-checked by Dr Lee Lip Seng, general surgeon at LS Lee Surgery, Mount Elizabeth Novena Specialist Centre, Singapore.
About the Doctor
Keyhole surgery, also known as laparoscopic surgery, is a minimally invasive surgical technique used in various medical fields, including the treatment of liver cancer. This article explores the diagnosis of liver tumors, criteria for surgical removal, treatment modalities for liver cancer, and the specific benefits of laparoscopic surgery.
1. Liver Tumor: Benign or Malignant?
Determining whether a liver tumor is benign or malignant is crucial for guiding treatment strategies. The diagnosis involves a combination of imaging studies, blood tests, presence of risk factors for liver cancer and biopsy.
(a) Imaging Studies
Imaging modalities such as ultrasound, computed tomography (CT), and magnetic resonance imaging (MRI) are the first steps in evaluating liver lesions. These techniques help in assessing the size, location, and characteristics of the tumor, providing valuable clues about its nature.
(b) Biopsy
A biopsy involves extracting a small tissue sample from the liver tumor under the guidance of imaging techniques. The sample is then examined under a microscope to determine the presence of cancer cells. This method is considered the gold standard for diagnosing liver cancer. However, this is not always performed due to the risk of tumor seedings and the spread of cancer when the biopsy is performed.
(c) Blood Tests
Blood tests, including the measurement of alpha-fetoprotein (AFP) levels, can support the diagnosis of liver cancer. Elevated AFP levels are often associated with hepatocellular carcinoma (HCC), the most common type of liver cancer. On the other hand, patients with cancer spread from the colon to the liver commonly have raised carcinoembryonic antigen (CEA).
(d) Risk Factors
The risk factors for liver cancer (HCC) include any conditions that can cause liver scarring or hardening resulting in liver cirrhosis (e.g. Hepatitis B infection, alcoholic liver cirrhosis and fatty liver).
2. Criteria for Surgical Removal in Liver Cancer
The selection of liver cancer patients for surgical removal is a critical and highly specific process, influenced by a detailed assessment of the cancer’s characteristics, the patient’s overall liver function, and the presence or absence of metastasis. Below are the refined criteria focusing explicitly on liver cancer:
(a) Type and Stage of Cancer
- Hepatocellular Carcinoma (HCC): Surgical resection is commonly considered for patients with early-stage HCC. This is because early-stage HCC is often localized and can be completely removed with surgery.
- Metastatic Liver Cancer: In certain cases where the liver cancer has originated from another primary site (metastatic liver cancer), surgery might still be an option if the cancer is limited to a few small areas in the liver and the primary cancer is under control.
(b) Liver Function
- Adequate Liver Reserve: Successful liver surgery requires remaining liver tissue to be sufficient to support life. This is often assessed using the Child-Pugh score, which evaluates liver function based on total bilirubin, serum albumin levels, prothrombin time, the presence of ascites, and encephalopathy. Only patients with good liver function (Child-Pugh A) are typically considered for surgery. Adequate liver reserve requires both good liver function and adequate future liver remnant (i.e. adequate remnant liver volume after resection)
(c) Tumor Size and Location
- Operable Tumors: Successful tumor resection needs to ensure cancer is removed completely and the patient still has adequate future liver remnant. Patients with no liver cirrhosis and good liver function can survive even with only 30% of future liver remnant.
- Vascular Invasion: The absence of major vascular invasion (e.g. involvement of the main portal vein, hepatic artery or inferior vena cava) is crucial. Tumors that encase or invade major blood vessels are often deemed inoperable due to the higher risk of complications.
(d) Absence of Widespread Disease
- Localized Disease: Surgery is considered most effective for patients whose cancer has not spread beyond the liver. This determination is typically made using advanced imaging techniques, such as PET scans or CT scans. These scans help to ensure that there is no distant metastasis, which would generally preclude the benefit of surgical removal of the liver tumor.
3. Treatment Modalities for Liver Cancer
Liver cancer, including primary forms such as hepatocellular carcinoma (HCC) and secondary (metastatic) cancers, requires a multifaceted approach to treatment. The choice of therapy depends on several factors, including the stage of the cancer, the overall liver function, and the health status of the patient. Here is a more detailed look at the treatment options specifically tailored for liver cancer:
(a) Surgical Resection
This involves the surgical removal of the cancerous part of the liver. It is most effective in patients with localized tumors and good liver function, without significant cirrhosis or other liver diseases. Resection is considered curative for small, well-defined tumors that have not invaded blood vessels or spread outside the liver.
(b) Liver Transplantation
Transplantation offers hope for patients with early-stage liver cancer who have severe liver dysfunction, typically due to underlying cirrhosis. The criteria for transplantation in liver cancer patients include the UCSF criteria. This approach aims to remove all cancerous cells and replace the liver with a healthy one, potentially curing the cancer and the liver disease.
(c) Ablation Therapy
Ablation destroys liver tumors without removing them. Techniques like radiofrequency ablation (RFA) and microwave ablation (MWA) use heat to kill cancer cells. Ablation is suitable for patients with small tumors (typically less than 3 cm) who may not be candidates for surgery due to their location within the liver or because of poor liver function.
(d) Embolization Therapy
This method targets tumors’ blood supply, essential for their growth and survival. Transarterial chemoembolization (TACE) combines embolization with chemotherapy, directly delivering cancer-fighting drugs to the liver tumor and blocking its blood supply. Another form, radioembolization (Y90), uses tiny radioactive beads to deliver radiation directly to the tumor. These approaches are beneficial for controlling tumor growth, especially in cases where surgery is not feasible.
(e) Targeted Therapy and Immunotherapy
Targeted therapies act on specific molecular targets associated with cancer cells, such as sorafenib, which is approved for advanced HCC. These drugs can stop the growth and spread of cancer cells while minimizing damage to healthy cells. Immunotherapy, like the checkpoint inhibitors nivolumab and pembrolizumab, boosts the body’s immune system to fight cancer. These treatments are options for advanced liver cancer, often used when the cancer has not responded to other treatments.
(f) Chemotherapy
Traditional chemotherapy, which uses drugs to kill cancer cells, has a limited role in treating liver cancer due to its effectiveness and the potential for liver damage. However, hepatic artery infusion (HAI) chemotherapy delivers chemotherapy drugs directly into the liver, targeting cancer cells more precisely and reducing systemic side effects. This technique may be used for advanced liver cancer or when other treatments are not suitable.
Each of these treatments has its benefits and potential risks, and the best approach depends on individual patient factors. A multidisciplinary team of specialists, including hepatologists, oncologists, and surgeons, typically collaborates to create a personalized treatment plan for each patient with liver cancer.
4. Benefits of Laparoscopic Surgery for Liver Cancer
Laparoscopic surgery, specifically tailored for the treatment of liver cancer, provides a range of advantages when compared to the traditional open hepatectomy.
(a) Enhanced Recovery and Reduced Postoperative Discomfort
Laparoscopic liver surgery involves making several small incisions rather than one large opening. This minimally invasive approach causes less post-operative pain, faster recovery, use less analgesia and minimise the risk of medication-related side effects.
(b) Minimized Hospital Stay Duration
One of the most immediate benefits observed with laparoscopic liver surgery is the reduced length of hospital stay. Since the procedure is less invasive, patients recover more quickly and are discharged earlier, thereby reducing potential hospital-acquired infections.
(c) Decreased Risk of Surgical Complications
The magnification provided by laparoscopic instruments allows for better visualisation and precision, with lower potential risk of complications such as bleeding, infections and incisional hernias associated with larger incisions in open surgery.
(d) Superior Cosmetic Results
Given that liver cancer surgery can be a major procedure, the prospect of minimal scarring is a significant advantage. Laparoscopic surgery for liver cancer uses small incisions, typically no more than a few centimeters in length, which result in minimal scarring. This aspect is particularly valued by patients, as it lessens the physical reminders of their surgery and cancer experience, contributing positively to emotional and psychological recovery.