(2) Degenerative lumbar spondylosis – This condition refers to the degenerative changes affecting the facet joints of the spine, as well as the formation of osteophytes (bone spurs) and thickened ligaments in the spinal column. It occurs because of chronic strain or trauma.
(3) Disc prolapse – Intervertebral disc prolapse is the protrusion of the soft inner material of the spinal disc, which then compresses the nerve root, often resulting in back pain, leg pain, numbness, and muscle weakness.
Treatment Options for Back Pain
When back pain in older adults becomes severe or significantly affects the quality of life, various treatment options are available. These options aim to reduce pain, improve mobility and neurologic deficits, and address the underlying causes, including:
(1) Medications – Nonsteroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, and neuropathic pain medications can help manage back pain and leg symptoms. However, it is crucial to consult a healthcare professional before starting any medication regimen.
(2) Epidural, nerve block and facet joint injections, and nucleoplasty of the intervertebral disc – these are different types of injections which can relieve back pain and neuropathic pain. In some cases, radio-frequency ablation (RFA) may be used to de-sensitize the affected nerves.
Photo 1: MRI lumbar spine showing disc prolapse and spondylolisthesis at L4-5 level
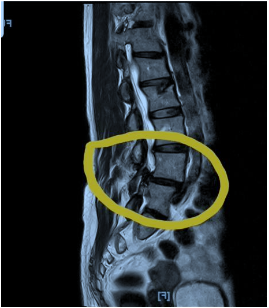
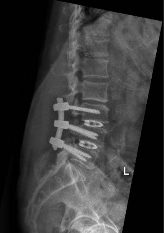
Photo 2: Xray showing 2-level lumbar spine fusion L3-5 level
(3) Surgery
(a) Decompression Surgery – for cases where the pain has become chronic and persistent, and with neurologic deficits affecting the legs, bladder or bowel, decompression surgery may be required to relieve pressure on the compressed nerves or spinal cord. The part of the bone or disc that is causing the nerve impingement is removed.
(b) Spinal Fusion – for cases where there is spinal instability, or where extensive bone decompression has to be done, this procedure will stabilise the spine, using titanium screws and rods to fuse two or more vertebrae together. Back pain is reduced when the spine is more stable and nerve pain is relieved by adequate decompression.
Consulting with experienced medical doctors who manage spine care is essential to get the correct treatment for better outcomes.