Urology
Who is Suitable to do Focal Therapy for Prostate Cancer?
Focal therapy for prostate cancer is an emerging treatment option that selectively targets cancerous areas within the prostate while preserving surrounding healthy tissue
This article has been fact-checked by Dr Chong Kian Tai, urologist at Surgi-TEN Specialists, Farrer Park Hospital, Singapore.
About the Doctor
Focal therapy for prostate cancer is an emerging treatment option that selectively targets cancerous areas within the prostate while preserving surrounding healthy tissue. This approach aims to minimise the side effects commonly associated with traditional treatments, such as radical prostatectomy surgery or whole-gland radiotherapy, which can lead to urinary incontinence, impotence, erectile dysfunction or urinary difficulties.
However, not all prostate cancer patients are candidates for focal therapy. Determining suitability requires a thorough evaluation of multiple factors, including cancer stage, tumor characteristics, and overall health.
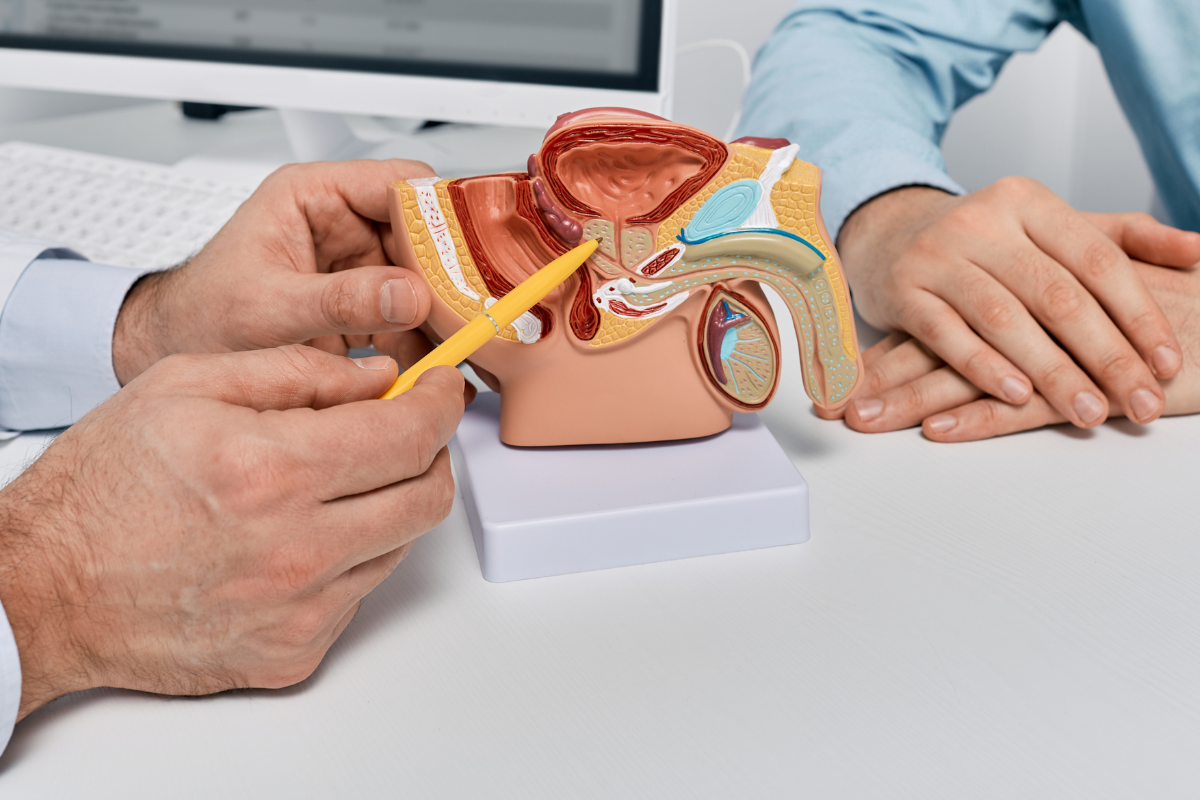
Understanding Focal Therapy
Focal therapy utilises advanced imaging and precision-targeting techniques to destroy cancerous tissue while sparing the rest of the prostate. Unlike traditional treatments that treat the entire prostate gland, focal therapy seeks to eliminate only the affected areas, reducing the risk of damage to nearby structures.
Techniques Used in Focal Therapy for Prostate Cancer
Several methods are used in focal therapy, each with unique mechanisms for destroying cancerous tissue:
- High-Intensity Focused Ultrasound (HIFU): Uses ultrasound waves to generate heat and destroy cancer cells in targeted prostate areas.
- Irreversible Electroporation (IRE): Also called the NanoKnife procedure, this technique uses electrical pulses to disrupt cancer cell membranes, leading to cell death to kill cancer cells.
- Cryotherapy: Involves freezing cancerous tissue with extremely cold gases, causing cell death while preserving healthy tissue.
- Laser Ablation: Uses high-intensity laser energy to vaporize cancerous cells, limiting damage to surrounding structures.
- Focal Brachytherapy: A form of radiation therapy that places radioactive seeds in a targeted manner within the prostate rather than treating the entire gland.
These treatments rely on advanced imaging techniques such as multiparametric MRI scans (mpMRI) and targeted prostate biopsies to locate cancerous regions with higher precision and accuracy, ensuring that treatment is applied only where necessary.
Ideal Candidates for Focal Therapy
Focal therapy is most effective for prostate cancer patients who meet specific criteria. The ideal candidates generally have low- to intermediate-risk disease, confined to a limited area within the prostate. Several factors determine eligibility:
1. Low-Risk and Intermediate-Risk Prostate Cancer
- Patients with a Gleason score of 6 or 7, with grade group 1 to 3 cancers (which indicates less aggressive cancer) are the best candidates.
- Those with high-risk or more aggressive cancers (Gleason score 8-10, with grade group 4 or 5 cancers) are not suitable, as their cancer is more likely to recur or spread.
2. Tumors Confined to the Prostate
- The effectiveness of focal therapy depends on whether the cancer is restricted to one or a few distinct areas within the prostate.
- Advanced imaging techniques such as multiparametric MRI (mpMRI) and targeted prostate biopsies help identify the exact cancer location and size.
3. PSA Levels Below a Certain Threshold
- Candidates typically have a prostate-specific antigen (PSA) level of 20 ng/mL or lower.
- Higher PSA levels may indicate a more aggressive or widespread disease, making focal therapy less effective.
4. No Evidence of Metastasis
- Focal therapy is only suitable for patients whose cancer is localized and has not spread to lymph nodes, bones, or other distant areas.
- Whole-body imaging may be required to confirm that there are no signs of metastasis.
5. Previous Prostate Radiotherapy but Cancer Recurs
- Men who have cancer recurring after undergoing previous radiation therapy can have successful focal therapy.
- Recurrent prostate cancer must be confined within the prostate gland to be suitable for focal therapy
6. Patients Seeking a Less Invasive Treatment
- Men who prefer to avoid the potential side effects of surgery or whole-gland prostate radiation may find focal therapy a more attractive option.
- However, men need to understand and accept the possibility of additional treatments in the future.
Who May Not Be a Good Candidate?
While focal therapy offers a promising treatment approach, it is not suitable for all prostate cancer patients. Certain conditions and cancer characteristics can make this approach ineffective or inappropriate.
1. High-Risk or Aggressive Tumors
- Patients with Gleason scores of 8-10, with grade group 4 or 5 cancers, typically have more aggressive cancers that are more likely to recur.
- These patients require more comprehensive treatment options, such as radical prostatectomy with bilateral pelvic lymph node surgery, or whole-gland radiation therapy in addition to hormone therapy.
2. Widespread Cancer in Multiple Extensive Areas of the Prostate
- If cancer is spread outside the capsule of the prostate, focal therapy may leave untreated areas, leading to recurrence.
- More aggressive approach may be recommended for multifocal or bilateral tumours based on the cancer location.
3. Very High PSA Levels
- Patients with PSA levels significantly above 20 ng/mL are more likely to have extensive disease that cannot be effectively treated with focal therapy alone.
- Additional diagnostic tests, such as bone scans or PET-CT scans, may be needed to determine if the cancer has spread.
4. Men Who Want a Single Definitive Treatment
- Some patients prefer a one-time treatment option that eliminates cancer with minimal risk of recurrence, and also accept the potential side effects of traditional treatment.
- Focal therapy for prostate cancer may require additional procedures if cancer returns, in order to have less side effects, less urine incontinence, or less erectile dysfunction.
Conclusion
Focal therapy for prostate cancer is an exciting and innovative treatment option for men with localized, low-risk to intermediate-risk prostate cancer. It offers the advantage of preserving urinary function with better quality-of life, while minimising side effects such as urinary incontinence and erectile dysfunction. However, patient selection is crucial for achieving the best outcome. Candidates must have organ-confined, less-aggressive tumours, an acceptable PSA level, and no evidence of cancer spread.